The Aerobic Ceiling: Why VO₂ Max is the Single Best Predictor of Longevity
An evidence-based deep dive into cardiorespiratory fitness and all-cause mortality.
Michael Donovan, PhD
3/17/202617 min read
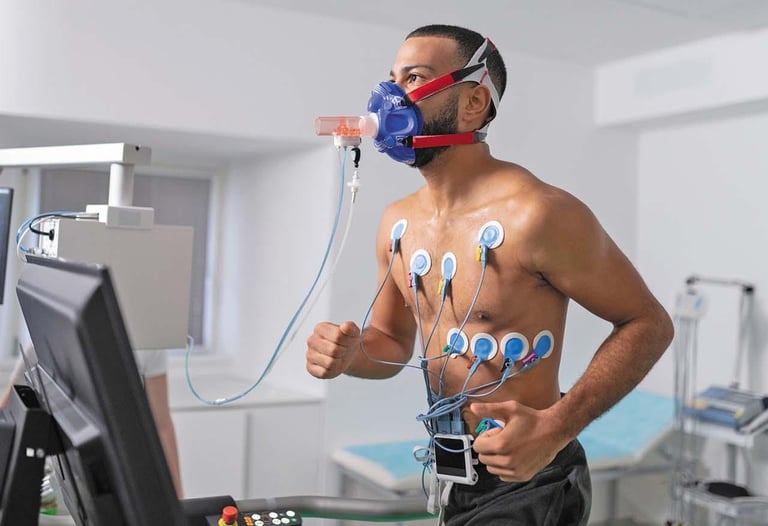
Table of Contents
1. Introduction: What Is VO₂ Max — And Why Should You Care?
2. The Evidence Base: Three Studies That Changed the Conversation
3. The Physiology of Longevity: Why Fitness Extends Life
4. Addressing the "Elite" Threshold: How High Is High Enough?
5. The Steel-Man: A Serious Look at the Opposing Evidence
6. Practical Application: Testing, Training, and Taking Action
7. Conclusion: The Most Powerful Modifiable Risk Factor You're Ignoring
1. Introduction: What Is VO₂ Max — And Why Should You Care?
There is a number — a single physiological metric — that predicts your risk of dying from nearly any cause better than whether you smoke, whether you have diabetes, or whether your blood pressure is controlled. That number is your VO₂ max.
VO₂ max, or maximal oxygen uptake, is the maximum rate at which your body can consume oxygen during intense exercise. It is typically expressed in milliliters of oxygen per kilogram of body weight per minute (ml/kg/min). The higher the number, the more efficiently your cardiovascular system, lungs, and muscles work together under stress. In performance science, it has long been the gold standard for measuring aerobic capacity. But in longevity medicine, it is emerging as something even more consequential: the single most powerful predictor of all-cause mortality.
Before we examine the evidence, a critical distinction is worth establishing. Most longevity conversations center on lifespan — the total number of years you live. But what arguably matters more is healthspan, or what we might call your functional span: the years during which you are physically capable, cognitively sharp, and genuinely independent. A person who lives to 90 but spends the last 15 years unable to climb stairs or carry groceries has not necessarily won. The goal is to compress the period of decline — to maintain function for as long as possible and to delay the point at which the body begins to fail.
VO₂ max sits at the center of this conversation because it is, in many ways, a direct measurement of your physiological reserve. Think of it as the ceiling of your aerobic engine. If your ceiling is high, ordinary activities — climbing stairs, carrying luggage, playing with grandchildren — consume only a fraction of your maximum capacity. You have headroom. As we age, that ceiling drops, and activities that were once easy begin to approach your maximum effort. The higher you build that ceiling in your 40s, 50s, and 60s, the more runway you preserve before ordinary life becomes exhausting.
Key Definition: VO₂ max is the maximum rate of oxygen consumption during maximal exertion. Units: ml/kg/min. It represents the ceiling of your aerobic engine and declines approximately 10% per decade after age 25, though this decline is substantially blunted by regular aerobic training.
What the clinical data now tell us — from cohort studies spanning hundreds of thousands of participants — is that this ceiling does not merely predict athletic performance. It predicts whether you will be alive in five, ten, and twenty years.
2. The Evidence Base: Three Studies That Changed the Conversation
The relationship between cardiorespiratory fitness (CRF) and mortality is among the most replicated findings in cardiovascular medicine. But three studies in particular deserve close attention — both for their scale and for the specificity of their conclusions.
2.1 The Mandsager / Cleveland Clinic Study (2018)
Published in JAMA Network Open in 2018, the study led by Kyle Mandsager and colleagues at the Cleveland Clinic is perhaps the most cited piece of evidence on fitness and longevity. The researchers retrospectively analyzed data from 122,007 patients who underwent exercise treadmill testing between 1991 and 2014.
Patients were stratified into five fitness categories based on their peak exercise capacity (measured in METs — metabolic equivalents): Low, Below Average, Above Average, High, and Elite. The Elite tier comprised the top 2.5% of performers for their age and sex. The study then tracked all-cause mortality over a median follow-up of 8.4 years.
The findings were striking:
• Low fitness was associated with the highest risk of death, used as the reference group.
• Elite fitness was associated with a roughly 5-fold lower risk of all-cause mortality compared to the Low fitness group.
• The survival benefit of moving from Low to Above Average fitness was comparable to, or greater than, quitting smoking, treating hypertension, or controlling type 2 diabetes.
• Crucially, the researchers found no upper limit — there was no point at which higher fitness began to harm longevity. The dose-response curve was monotonically favorable.
• Among patients aged 70 and above, Elite fitness was associated with an approximately 5× survival advantage over Low fitness — suggesting the benefit does not diminish with age.
The Mandsager et al. (2018) conclusion: "Cardiorespiratory fitness is inversely associated with long-term mortality with no observed upper limit of benefit. Extreme cardiorespiratory fitness was associated with the greatest survival."
The study is not without limitations. It was observational and retrospective — patients were referred for treadmill testing, which may introduce selection bias (these are people already concerned about their cardiac health). Causality cannot be formally established. However, the sheer size of the cohort, the duration of follow-up, and the consistency of the dose-response relationship make the data difficult to dismiss.
2.2 The "4-Minute Mile" Study (2024): Debunking the Extreme Exercise Hypothesis
A persistent concern in sports medicine has been the so-called Extreme Exercise Hypothesis — the idea that prolonged, very high-intensity cardiovascular training might paradoxically harm the heart. The hypothesis draws on data showing elevated rates of coronary artery calcification (CAC) in veteran endurance athletes and some evidence of right ventricular dysfunction in those completing multiple Ironman triathlons.
A landmark 2024 study addressed this concern head-on by examining a rare natural experiment: what happens to individuals who run a sub-4-minute mile — among the most demanding athletic achievements in human history — across their entire lifespan? The research, which tracked former elite milers over decades, found that these individuals lived significantly longer than age- and sex-matched controls from the general population, with substantially lower rates of cardiovascular disease and cancer mortality.
The key finding was not merely that these men survived longer — it is that they survived longer despite a lifetime of extremely high training volumes and intensities. If the Extreme Exercise Hypothesis held, we would expect to see mortality converging or even reversing at the highest fitness levels. It did not. The sub-4-minute milers demonstrated that the fitness-longevity relationship extends into domains of performance most clinicians would consider extraordinary.
This does not mean every individual should train like an elite middle-distance runner. But it does significantly undercut the argument that high aerobic fitness is dangerous. The evidence, taken together, suggests that the heart adapts beneficially to high aerobic demand — developing what is known as the "athlete's heart," characterized by enlarged ventricular chambers, improved stroke volume, and enhanced diastolic function.
2.3 The Kokkinos Veterans Study: Quantifying the Dose
Peter Kokkinos and colleagues have published extensively on the fitness-mortality relationship using the Veterans Affairs health system as their data source — a uniquely valuable population given its size, longitudinal tracking, and relatively controlled demographics. Across multiple analyses encompassing hundreds of thousands of veterans, a consistent finding emerges:
Each 1 MET increase in peak exercise capacity is associated with approximately a 13–15% reduction in all-cause mortality risk. This relationship holds across age groups, sexes, and the presence or absence of cardiovascular disease at baseline.
To contextualize what 1 MET means practically: 1 MET is approximately the energy expenditure of sitting quietly. Walking briskly is roughly 3–4 METs. Jogging at a comfortable pace is 7–8 METs. Elite aerobic athletes can sustain efforts at 15–20+ METs. Moving from 8 METs to 10 METs of peak exercise capacity — a difference achievable through several months of structured training — corresponds to a 26–30% reduction in mortality risk.
The Kokkinos data are particularly useful because they allow us to think about fitness as a modifiable drug. Unlike genetics or age, peak exercise capacity can be meaningfully changed through training. The question shifts from "is fitness important?" to "how much fitness can I acquire, and how quickly?"
Summary: Risk Comparison Table
The following table contextualizes the magnitude of low cardiorespiratory fitness as a mortality risk factor relative to traditional clinical risk factors.
Risk Factor Relative Mortality Risk Modifiable? Evidence Quality
Active Smoking 2×–3× Partially (cessation) High
Type 2 Diabetes 2×–3× Partially (management) High
Hypertension 1.5×–2× Partially (medication) Moderate
Low Cardiorespiratory Fitness 5× Yes — fully modifiable Very High
Data adapted from Mandsager et al. (2018), Kokkinos et al. (multiple), and comparative risk analyses published in the European Heart Journal and JAMA.
3. The Physiology of Longevity: Why Fitness Extends Life
Epidemiological data tell us that fitness predicts longevity. But the question of mechanism matters — both scientifically and practically. Understanding why high VO₂ max extends life helps us understand what we are actually training when we train aerobically, and it makes the clinical data feel less like statistical abstraction and more like biology you can act on.
3.1 Mitochondrial Density and the Engine of Metabolism
Mitochondria are the organelles responsible for producing adenosine triphosphate (ATP) — the universal energy currency of the cell. Every aerobic process in your body, from walking upstairs to healing a wound to generating a heartbeat, depends on mitochondrial function. What most people do not appreciate is that mitochondrial density — the number and efficiency of mitochondria per unit of muscle tissue — is one of the most trainable aspects of human physiology.
Sustained aerobic exercise, particularly at intensities that keep you near your lactate threshold (often called Zone 2 training), is the most potent stimulus for mitochondrial biogenesis — the creation of new mitochondria. High VO₂ max individuals do not just have more mitochondria; their mitochondria also tend to be more functionally efficient, with higher activity of key oxidative enzymes and tighter coupling between electron transport and ATP synthesis.
The longevity implications are profound. Mitochondrial dysfunction is implicated in virtually every major age-related disease: Alzheimer's, Parkinson's, type 2 diabetes, cardiovascular disease, and cancer. Cells with healthy, abundant mitochondria are better at managing oxidative stress, signaling appropriate apoptosis (programmed cell death), and maintaining metabolic flexibility — the ability to switch between fat and glucose as fuel sources. High aerobic fitness essentially up-regulates the cellular machinery that keeps aging at bay.
3.2 Stroke Volume and Cardiac Reserve
The heart is a pump, and like any pump, it is characterized by its output. Cardiac output — the volume of blood ejected per minute — is the product of heart rate and stroke volume (the volume ejected per beat). At rest, most adults have a cardiac output of roughly 5 liters per minute. During maximal exertion, trained individuals can achieve outputs of 20–40 liters per minute, driven primarily by dramatic increases in stroke volume.
Endurance training enlarges the left ventricle and increases its compliance — its ability to stretch and fill. This produces what is known as the "athlete's heart": a larger, more efficient pump that can deliver substantially more blood per beat. The resting heart rates of highly trained aerobic athletes (40–50 bpm, versus 70–80 bpm in sedentary individuals) are a direct expression of this adaptation. Each beat delivers more blood, so fewer beats are needed.
The concept of cardiac reserve — the difference between resting and maximal cardiac output — is critical. A high cardiac reserve means that in ordinary life, you are operating far from your ceiling. Activities of daily living require only a small fraction of your maximum output. This reserve is not merely an athletic luxury. It becomes the difference between an 80-year-old who can climb two flights of stairs and one who cannot — and the research consistently shows that inability to perform basic physical tasks is a leading predictor of disability, hospitalization, and death.
3.3 Endothelial Health and Vascular Elasticity
The endothelium — the single-cell-thick lining of every blood vessel in your body — is not passive scaffolding. It is a metabolically active organ that regulates vascular tone, inflammation, clotting, and the passage of substances between blood and tissue. Endothelial dysfunction is among the earliest pathological changes in atherosclerosis and is associated with hypertension, insulin resistance, and impaired organ perfusion.
Aerobic exercise is one of the most powerful stimuli for endothelial health. The shear stress of increased blood flow during exercise triggers the release of nitric oxide (NO), a vasodilatory molecule that relaxes smooth muscle in vessel walls, reduces blood pressure, and has anti-inflammatory and anti-thrombotic effects. Over time, regular aerobic training produces lasting improvements in endothelial function, measurable as increased flow-mediated dilation of the brachial artery.
Vascular elasticity — the ability of arteries to expand and contract with each heartbeat — declines with age and atherosclerosis, contributing to systolic hypertension and increased cardiac workload. Regular endurance training preserves and partially restores arterial compliance. High-fitness individuals consistently show more elastic central arteries than age-matched sedentary controls, and this difference becomes more pronounced with advancing age.
3.4 Metabolic and Inflammatory Effects
Beyond these structural adaptations, high cardiorespiratory fitness is associated with a cluster of metabolic improvements that independently reduce disease risk:
• Insulin sensitivity: Aerobic training enhances glucose transporter (GLUT4) expression in skeletal muscle, improving insulin-mediated glucose uptake and reducing fasting insulin. This is independent of weight loss.
• Lipid metabolism: High fitness is associated with elevated HDL cholesterol, reduced triglycerides, and a shift toward larger, less atherogenic LDL particle size.
• Systemic inflammation: Chronic exercise reduces circulating inflammatory markers including C-reactive protein (CRP), interleukin-6 (IL-6), and tumor necrosis factor-alpha (TNF-α). Persistent low-grade inflammation is a common pathway in atherosclerosis, neurodegeneration, and many cancers.
• Autonomic tone: Fit individuals show greater parasympathetic (vagal) tone, manifest as higher heart rate variability (HRV). Vagal tone is a strong independent predictor of cardiovascular mortality.
4. Addressing the "Elite" Threshold: How High Is High Enough?
One of the most important — and often misunderstood — findings from the fitness-mortality literature is the nature of the dose-response curve. Many clinicians and patients operate under the assumption that moderate exercise is sufficient: that reaching an "average" fitness level provides most of the benefit and that further improvement yields diminishing returns. The data suggest otherwise.
The Mandsager Cleveland Clinic study and subsequent analyses reveal a dose-response relationship that is notably non-linear. The largest absolute mortality reduction occurs when moving from the Low to Below Average tier — a clinically massive improvement achievable even through modest lifestyle changes. But the survival benefit does not plateau at Average or Above Average fitness. It continues to increase monotonically through the High tier and into the Elite tier (top 2.5% of age-sex matched peers), with no observed inflection point where higher fitness becomes neutral or harmful.
VO₂ Max Fitness Tiers + Relative Mortality Risk
Fitness Tier
VO₂ Max (Men, 40–49)
All-Cause Mortality Risk
Low (Bottom 25%)
< 34 ml/kg/min (men)
Reference (1×)
Below Average
34–42 ml/kg/min
~2× relative risk
Average
43–52 ml/kg/min
~1.5× relative risk
Above Average
53–62 ml/kg/min
~1.3× relative risk
High
63–72 ml/kg/min
~1.15× relative risk
Elite (Top 2.5%)
> 73 ml/kg/min
Lowest - reference target
Note: Values are approximate and age-sex dependent. "Men, 40–49" used as reference. Derived from Mandsager et al. (2018) and Kokkinos et al. data.
This has a practical implication that is counterintuitive to many: the person in the 60th percentile of fitness for their age is not done. Moving from the 60th to the 80th or 95th percentile continues to provide survival benefit. The goal is not merely to escape the bottom quintile — it is to build the largest aerobic ceiling you can, given your time, recovery capacity, and physiology.
This is particularly relevant for individuals who have already made significant lifestyle improvements. A former smoker who now walks 30 minutes daily has taken a meaningful step. But if they have the capacity to progress to structured aerobic training, the data suggest they should — not from perfectionism, but because the mortality curves clearly favor higher fitness at every level.
The concept of the "Aerobic Ceiling" matters here: the higher you build it in your 40s and 50s, the more physiological buffer you carry into your 70s and 80s, when the age-related decline in VO₂ max (approximately 10% per decade, but substantially blunted by training) may otherwise bring you below the functional threshold for independence.
5. The Steel-Man: A Serious Look at the Opposing Evidence
Intellectual honesty requires engaging with the strongest version of the opposing argument. In this case, that argument centers on cardiac fibrosis and atrial fibrillation in veteran endurance athletes — and it deserves a careful hearing.
The Extreme Exercise Hypothesis is not without empirical support. A series of studies over the past two decades have documented findings in veteran endurance athletes — individuals who have completed decades of high-volume training and racing — that are at minimum worth attention:
5.1 Coronary Artery Calcification in Master Athletes
Several cross-sectional studies have found that male veteran endurance athletes (particularly marathon runners and cyclists aged 50 and older) show higher coronary artery calcium (CAC) scores than age-matched sedentary controls. CAC is a well-validated marker of atherosclerosis and is independently associated with cardiovascular events.
At first glance, this seems to directly contradict the fitness-longevity relationship. However, a critical nuance emerges from the data: CAC type matters. In veteran athletes, elevated CAC tends to reflect dense, calcified plaques — the kind that are more stable and less likely to rupture and cause acute myocardial infarction — rather than the mixed or soft plaques seen in sedentary individuals with similar total calcium scores. This distinction is clinically meaningful: it is the soft, lipid-rich plaque that tends to rupture and cause heart attacks.
5.2 Atrial Fibrillation in Veteran Endurance Athletes
This is the most substantiated concern in the literature, and it merits direct engagement. Multiple well-conducted studies have demonstrated that long-term, high-volume endurance exercise — particularly in men who engaged in decades of intense training — is associated with an approximately 2–5 fold higher risk of atrial fibrillation (AF) compared to moderately active or sedentary controls.
The proposed mechanism involves structural and electrical remodeling of the atria: chronic volume overload leads to atrial enlargement and fibrosis, creating the substrate for re-entry circuits that drive AF. This is not a trivial concern — AF is the most common cardiac arrhythmia, is associated with stroke, heart failure, and cognitive decline, and can be highly symptomatic.
The most honest reading of the data acknowledges this tension:
• High aerobic fitness unambiguously reduces all-cause mortality, cardiovascular mortality, and cancer mortality across large populations.
• Extreme training volumes in male veteran athletes (tens of thousands of lifetime training hours) may increase AF risk — a specific arrhythmia risk that is real and not entirely explained away.
• The populations at highest AF risk are those who have been training at very high volumes for decades — not individuals building their VO₂ max through structured moderate-to-vigorous exercise.
• Women appear to have substantially lower risk of exercise-associated AF than men, for reasons that are not fully understood.
5.3 Putting the Opposing Evidence in Context
The key question is not whether extreme training volumes carry any risk — they appear to carry a modest, specific one (primarily AF in male veteran athletes). The question is whether that risk outweighs the profound, broad, and consistent survival benefit of high cardiorespiratory fitness.
The balance of evidence strongly suggests it does not. Studies directly comparing all-cause mortality in veteran endurance athletes to sedentary controls consistently show that the athletes live longer, not shorter lives, despite the AF signal. AF is serious and manageable; the conditions that kill most people — cardiovascular disease, cancer, metabolic syndrome, and the physical decline associated with low fitness — appear substantially mitigated by high CRF.
A reasonable clinical translation: build the highest aerobic ceiling you can. If you are a male athlete considering training volumes of 15–20+ hours per week into your 60s and 70s, periodic cardiac monitoring (including rhythm surveillance) is prudent. But the response to AF risk is not to avoid aerobic exercise — it is to be thoughtful about training volume, recovery, and cardiac screening.
6. Practical Application: Testing, Training, and Taking Action
Understanding that VO₂ max predicts longevity is only useful if it motivates change. The practical questions are: how do you measure it, and how do you improve it?
6.1 Measuring Your VO₂ Max
There are several methods available, ranging from clinical-grade laboratory testing to consumer wearable estimates:
Gold Standard: Maximal Graded Exercise Test
A VO₂ max test performed in a sports medicine or cardiology laboratory with breath-by-breath gas analysis is the definitive measurement. The subject exercises on a treadmill or cycle ergometer at progressively increasing intensities while oxygen consumption and carbon dioxide production are measured directly. Results are highly accurate but require equipment, clinical supervision, and are typically not covered by insurance for healthy adults.
Clinical Approximation: Sub-Maximal Treadmill Test
The Bruce Protocol and modified Bruce Protocol are commonly used in clinical settings to estimate VO₂ max from peak METs achieved during a graded treadmill test. While not as precise as direct measurement, these protocols are validated against direct measurement and provide clinically meaningful stratification (the same tiers used in the Mandsager study were based on MET-based treadmill performance).
Field Test: The Cooper 12-Minute Run
Developed by Kenneth Cooper in 1968, this field test requires running as far as possible in 12 minutes. VO₂ max is estimated from the distance covered using a validated equation. The Cooper test is free, requires no equipment beyond a track or GPS, and provides a reasonably accurate estimate for healthy adults. It is not appropriate for deconditioned or cardiac-risk individuals without medical clearance.
Cooper Test Formula: VO₂ max (ml/kg/min) ≈ (distance in meters − 504.9) ÷ 44.73
Wearable Devices
Consumer fitness trackers from Garmin, Apple, Polar, and WHOOP now provide VO₂ max estimates derived from heart rate data during outdoor runs or structured workouts. Validation studies show these estimates are meaningful for tracking trends over time, though their absolute accuracy (typically ±3–5 ml/kg/min) is lower than laboratory testing. For most individuals, the trend line matters more than the precise number: if your estimated VO₂ max is climbing month over month, your training is working.
6.2 Training to Improve VO₂ Max
VO₂ max is trainable throughout the lifespan, though the rate of improvement varies with age, baseline fitness, and training structure. Two training modalities have the strongest evidence base for improving VO₂ max:
Zone 2 Training: Building the Aerobic Base
Zone 2 refers to exercise performed at an intensity where you can sustain a conversation but feel challenged — roughly 60–70% of maximum heart rate, or at the upper limit of fat oxidation as a fuel source. This intensity corresponds to the zone just below the first lactate threshold. Zone 2 training is the primary stimulus for mitochondrial biogenesis, fat oxidation capacity, and capillary density in muscle tissue.
Most longevity-focused training protocols recommend approximately 3–5 hours of Zone 2 per week as the aerobic foundation. This is work done at a moderate, sustainable intensity — not intervals, not maximal efforts, but sustained aerobic stress that drives foundational adaptations over weeks and months.
VO₂ Max Intervals (4×4 Protocol)
To specifically raise the ceiling — to increase VO₂ max itself — research strongly supports high-intensity interval training (HIIT) protocols that push the cardiovascular system to or near its maximal capacity. The best-validated protocol for improving VO₂ max is the Norwegian 4×4:
• 4 intervals of 4 minutes each at approximately 90–95% of maximum heart rate
• 3 minutes of active recovery (easy jogging or walking) between intervals
• Performed 1–2 times per week, in addition to Zone 2 base work
• Shown in randomized controlled trials to improve VO₂ max by 5–10% over 8–12 weeks
The 4×4 protocol was developed and studied extensively by Ulrik Wisløff and colleagues at the Norwegian University of Science and Technology, where it has been tested in healthy adults, cardiac rehabilitation patients, and heart failure populations — producing meaningful improvements in VO₂ max and downstream health markers in each group.
6.3 Setting a Target
Based on the Mandsager data, the longevity benefit begins to plateau meaningfully only in the Elite tier (top 2.5% for age and sex). A reasonable clinical target, particularly for individuals who are currently in the Low or Below Average categories, is to reach at minimum the Above Average tier. For those already there, continuing to build toward High or Elite remains beneficial.
Age-specific VO₂ max norms differ by sex. As a general reference point for men in their 40s, Above Average begins around 45–50 ml/kg/min; Elite begins around 55–60 ml/kg/min. For women in their 40s, the thresholds are approximately 38–42 ml/kg/min for Above Average and 48–52 ml/kg/min for Elite. Consulting published normative tables (or discussing with a sports medicine physician) provides a personalized benchmark.
7. Conclusion: The Most Powerful Modifiable Risk Factor You're Ignoring
The clinical case for VO₂ max as the primary longevity biomarker is, at this point, remarkably strong. Across cohorts totaling hundreds of thousands of participants, followed for years to decades, the evidence converges on a consistent finding: the higher your cardiorespiratory fitness, the lower your risk of dying from essentially any cause — cardiovascular disease, cancer, metabolic disease, and even all-cause mortality combined.
The magnitude of this effect is not subtle. The difference in mortality risk between the bottom quintile and the top 2.5% of fitness for age and sex — roughly a 5-fold reduction — exceeds the effect size of most pharmacological interventions in cardiology. We do not have a drug that produces this outcome. We have exercise.
Crucially, unlike most powerful mortality predictors — age, genetics, birth circumstances — cardiorespiratory fitness is modifiable. It responds to training at any age. Meaningful improvements in VO₂ max are achievable in individuals in their 60s, 70s, and even 80s. And unlike many preventive interventions, the benefits accrue quickly: measurable improvements in aerobic capacity typically emerge within 6–12 weeks of structured training.
The opposing evidence — particularly the signal of increased atrial fibrillation risk in male veteran endurance athletes with extreme lifetime training volumes — deserves acknowledgment, not dismissal. But placed in full context, it does not alter the fundamental conclusion. It refines it: build the highest aerobic ceiling you responsibly can, with appropriate monitoring if training volumes are very high.
The prescription is not complicated. It does not require racing, obsessing, or training to exhaustion. It requires consistency: 3–5 hours per week of Zone 2 aerobic work, supplemented by 1–2 sessions of higher-intensity intervals. Done consistently over months and years, this training will raise your VO₂ max, expand your cardiac reserve, improve your metabolic health, and — according to the best available clinical evidence — meaningfully extend both your lifespan and your functional span.
Fitness, in this sense, is not a lifestyle choice in the recreational sense of the term. It is a clinical intervention — arguably the most effective one available without a prescription. The data are in. The question is whether you will act on them.
Key References
1. Mandsager K, et al. "Association of Cardiorespiratory Fitness With Long-term Mortality Among Adults Undergoing Exercise Treadmill Testing." JAMA Netw Open. 2018;1(6):e183605.
2. Kokkinos P, et al. "Exercise Capacity and Mortality in Older Men: A 20-Year Follow-Up Study." Circulation. 2010;122(8):790–797.
3. Wisløff U, et al. "Superior Cardiovascular Effect of Aerobic Interval Training Versus Moderate Continuous Training in Heart Failure Patients." Circulation. 2007;115(24):3086–3094.
4. Merghani A, et al. "Prevalence of Subclinical Coronary Artery Disease in Masters Endurance Athletes." Eur Heart J. 2017;38(35):2622–2629.
5. Grimsmo J, et al. "High Prevalence of Atrial Fibrillation in Long-Term Endurance Cross-Country Skiers." Eur Heart J. 2010;31(19):2357–2363.
6. Cooper KH. "A Means of Assessing Maximal Oxygen Intake." JAMA. 1968;203(3):201–204.
7. Lavie CJ, et al. "Extreme Physical Activity and Cardiovascular Prognosis: Revisiting the J-Curve Hypothesis." Circulation. 2023.